Women’s access to emergency contraceptives key to avoiding unwanted pregnancies

Kalpana Acharya\Kathmandu: Ensuring sexual and reproductive health rights (SRHR) is considered an essential element to achieving universal health coverage by 2030, a commitment that countries have made to achieve by 2030. Part of delivering on SRHR-related goals and targets is widely believed to be through expanding the choices for women and girls to prevent unintended pregnancies.
However, in a setback to this commitment, many women have been experiencing contraception failure, missing taking oral contraceptive pills, or been forced to have sex against their will, says a renowned public health professor.
“For these women, emergency contraception (EC) is a safe and effective method that reduces the risk of pregnancy,” said Professor Angela Dawson who is associated with the Public Health at The Australian Center for Public and Population Health Research.
“However, many women remain unaware of this important option and in many countries in the Asia-Pacific region, access of EC is still limited and it largely remains a neglected contraception method,” she said speaking at the “Launch of the Asia Pacific Consortium for Emergency Contraception (APCEC)” during a virtual session of the ongoing 10th Asia Pacific Conference on Reproductive and Sexual Health and Rights (APCRSHR10).
APCRSHR is a biennial gathering of civil society, young people, academia, government, media, private sector, and development partners from the Asia region working on SRHR and its 10th edition is organized by Reproductive Health Association of Cambodia in partnership with UNFPA.
With its establishment, APCEC now aims to address this through advocacy efforts, knowledge dissemination and networking to improve evidence based policy and practice and access to EC in the region.
It is said that EC can prevent up to over 95% of pregnancies when taken within five days after intercourse. It can be used in situations like unprotected intercourse, concerns about possible contraceptive failure, incorrect use of contraceptives, and sexual assault.
It prevents pregnancy by preventing or delaying ovulation. It is not an abortifacient and not Teratogenic. There is low knowledge, myths and misunderstandings, misinformation, stigma and discrimination around EC.
During quarantine and lockdowns, rates of intimate-partner violence appear to have increased. Fear, service closures or restricted hours due to staff redeployment leads to less access to EC; uptake of regular contraception, and increases likelihood of unintended pregnancy; possible contraceptive failure.
















बसाइ नमिल्दा ढाड दुख्ने समस्या !
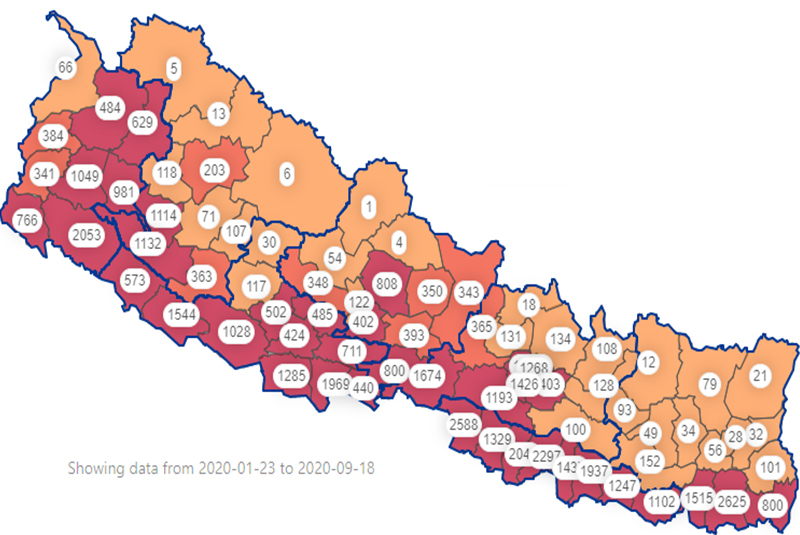
काठमाडौंमा १७ जना औंलोको बिरामी, सबै आयातित
स्वास्थ्य मन्त्रालयले भन्यो, सरकारी अस्पतालमा काम गर्ने अनि निजीको विज्ञापन गर्न कहाँ पाइन्छ ?
गर्मीमा तातो हावा ‘लू’ बाट कसरी जोगिने ?
राष्ट्रिय प्रत्यारोपण केन्द्र १२ वर्षमा : १२ सय ३१ जनाको मिर्गौला प्रत्यारोपण